Feline Diabetes
What is Diabetes?
Diabetes mellitus is a condition in which the body cannot properly produce or respond to the hormone insulin. This results in elevated levels of the sugar glucose in the blood, which is the main source of energy for the body.
Like the human body, the cells in a cat’s body need sugar in the form of glucose for energy. However, glucose in the blood requires insulin, a hormone produced by the pancreas, to “unlock” the door to cells. Insulin attaches to cells and signals when the time is right to absorb glucose. By absorbing glucose, cells in fat deposits, the liver, and the muscles get vital fuel while lowering levels of glucose in the blood.
In Type I diabetes, blood glucose concentrations are high because of a decrease in insulin production. In Type II diabetes, glucose levels are high because cells in the body do not respond appropriately to insulin. In both Type I and Type II diabetes, cells cannot access the nutrients they need even though there is plenty of sugar in the blood, because insulin can’t transport the sugar from the bloodstream into the cells that need it.
Cats with diabetes most commonly suffer from the Type II form of the disease. It is estimated that between 1:100 and 1:500 cats will be diagnosed with diabetes during their lifetime.
Risk Factors
The most important risk factors identified for the development of diabetes in cats include obesity, increasing age, physical inactivity, male gender, and the use of glucocorticoids (steroids) to treat other illnesses such as feline asthma. In some countries, Burmese cats appear to have a higher risk of developing diabetes than other breeds, but this may not be true in the United States.
Obese cats are up to four times more likely to develop diabetes than ideal weight cats, so the most important thing a cat owner can do to decrease their risk of developing diabetes is to maintain a healthy weight and encourage physical activity through daily play.
Clinical Signs
The two most common signs of diabetes noticed by owners at home are weight loss despite a good appetite and increased thirst and urination.
Weight loss may be noticed at home or during a routine examination with the veterinarian. In both Type I and Type II diabetes, the cells in the body are unable to absorb glucose from the blood and become starved of energy. To get the energy it needs, the body turns to other sources, breaking down fats and proteins to feed glucose-starved cells. This breakdown results in weight loss, despite an increased appetite.
Excessive thirst and urination can also signal diabetes in a cat. High levels of sugar in the blood can overwhelm the ability of the kidney to filter glucose, allowing sugar to “spill out” of the blood and into the urine. This high urine glucose concentration can actually pull excessive amounts of water into the urine, resulting in increased urine volume, increased urinary water loss, a propensity for dehydration, and a compensatory increase in thirst.
In rare cases of uncontrolled diabetes, cats may experience damage to the nerves in the hind limbs, resulting in a “plantigrade” stance of the hind limbs (walking or standing with their hocks on or close to the ground). This is not painful, and will often resolve with treatment.
Diagnosis
Your veterinarian will diagnose diabetes mellitus by demonstrating persistently elevated glucose levels in a cat’s blood and urine. This testing, along with consistent clinical signs, will lead to the diagnosis of diabetes.
A single blood glucose reading in a veterinary clinic may not be sufficient to diagnose diabetes in all cases. Cats can develop a short-term elevation in blood glucose as a response to stress, known as stress hyperglycemia. In these uncertain cases a lab test known as a fructosamine concentration can be helpful. This test gives a rough average of a cat’s blood glucose concentration over the last two weeks, so would not be affected by stress hyperglycemia.
Other tests will likely be recommended by the veterinarian to rule out other diseases which might be contributing to a cat’s clinical signs, such as a urinary tract infection, chronic kidney disease, pancreatitis or hyperthyroidism.
Treatment
The main goals of treatment for feline diabetes are:
- Restoring normal blood glucose concentrations
- Stopping or controlling weight loss
- Stopping or minimizing signs of increased thirst and urination
- Avoiding inappropriately low blood sugar due to treatment (hypoglycemia)
These goals are traditionally achieved through a combination of insulin and dietary therapy, though new oral medications may be a good treatment option for some cats. Treatment options should be discussed with the veterinarian based on each individual cat.
Insulin Therapy
Injectable insulin is a mainstay of treatment for feline diabetes and has generally been considered the standard of care for cats with this disease. There are multiple types of insulin preparations that can be used for cats in the treatment of diabetes, such as lente insulin (Vetsulin), ProZinc or glargine insulin. These types of insulin vary in cost, duration of action, and concentration, so it is important for an owner to discuss the pros and cons of each type with their veterinarian when deciding which insulin is best for their cat. It is also important to note that each insulin type has a specific syringe size (U-100 or U-40), so it is vital that a cat owner ensure that they are using the appropriate syringe for their cat’s insulin.
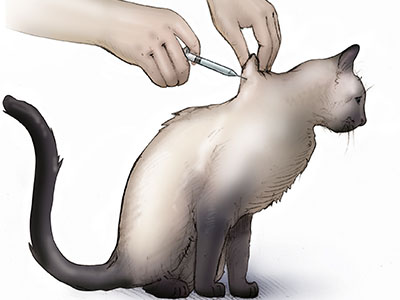
Insulin injections are given under the skin (subcutaneously) approximately every 12 hours. While giving injections may seem daunting, most owners can be taught to administer these injections at home quite easily and due to the very small needle size, cats tend to tolerate these injections very well. Though ideally injections should be spaced 12 hours apart, varying injection times by 1-2 hours when needed will not adversely affect a cats’ treatment.
Dietary Therapy
A diet low in carbohydrates has been shown to improve blood sugar regulation in diabetic cats. There are several prescription food options that are available in both wet and dry food forms, though feeding a wet-food only diet may be beneficial for many cats. For cats who are overweight when diagnosed with diabetes, slow, controlled weight loss under the close monitoring of a veterinarian is very important to achieve better control over blood glucose levels.
The optimal timing of meals for diabetic cats is controversial. Many veterinarians recommend feeding at the time of insulin injection to avoid a dangerous drop in blood glucose levels. However, there is no definitive evidence that the timing or frequency of meals in diabetic cats protects them from insulin-induced hypoglycemia. With a low carbohydrate diet, free choice feeding may be acceptable for cats who prefer to “graze” throughout the day, especially if a longer-acting insulin preparation is used. If food must be withheld for any reason, such as an anesthetic procedure, it is generally recommended to give 50 percent of the usual dose of insulin, with careful follow-up monitoring to ensure good glycemic control.
Oral Medications
In 2023, a new class of medications that are administered by mouth once daily was approved for the treatment of feline diabetes,. These medications, known as SGLT2 (sodium-glucose cotransporter 2) inhibitors, lower the concentration of glucose in the blood by increasing the amount excreted through the kidneys. These medications help improve the clinical signs of diabetes by lowering insulin resistance and reducing damage to the pancreas, allowing the cat to produce more of its own insulin. Because these treatments rely on the cat making at least some insulin on its own, it is not appropriate for every patient, and this treatment should be discussed with a veterinarian before starting. SGLT2 inhibitors are approved for treatment of newly-diagnosed diabetic cats who are otherwise healthy and have not been previously treated with any injectable insulin, and studies have shown these medications to be more than 80% effective at improving blood glucose control in appropriate patients.
Monitoring
Close monitoring by both the owner and the veterinarian is an essential part of treatment for a diabetic cat. Regular monitoring will help determine the ideal insulin dose for each cat as well as help avoid complications, such as hypoglycemia or uncontrolled diabetes and diabetic ketoacidosis. Regular assessments of weight, water intake, and appetite should be recorded to help determine if treatment goals are being met.
Blood glucose curves are the ideal way to monitor blood sugar regulation during treatment. During a blood glucose curve, the cat’s blood sugar will be checked right before receiving an insulin injection, and then every 1-4 hours throughout the day. This helps make sure that the average blood glucose is within an acceptable range, and that the value does not drop dangerously low at any time throughout the day. These assessments may need to be performed every few weeks when a cat is first diagnosed with diabetes in order to determine the appropriate dose of insulin, but can be spaced out further once the diabetes is more well-regulated. Even in a stable cat, blood glucose curves should still be performed every 3-4 months, as insulin needs can change over time.
Eventually, many cat owners can learn to perform blood glucose curves at home. This helps avoid stress hyperglycemia and inappetence experienced by many cats in the veterinary clinic, and can therefore give more accurate results. Blood can be collected at home from an ear vein or paw pad, and should be read on a blood glucose monitor that has been tested in cats. Alternatively, some veterinarians may utilize a continuous blood glucose monitoring system to help determine blood sugar concentrations at home. With this approach, a small monitor is implanted on the cat’s skin in the veterinary clinic, which stays in place and records blood glucose readings every few minutes for a few days up to two weeks. Though this can provide a lot of information without repeated needle pricks, not all cats will tolerate the monitor for long so it is not a viable option for all owners. It is very important that owners who monitor blood glucose readings at home do NOT change their cat’s insulin dose without discussing first with their veterinarian.
If performing a blood glucose curve is not an option, a fructosamine concentration can be used to get a rough estimate of blood sugar control over the last two weeks with a single blood draw. However, this is not an ideal way of monitoring a diabetic cat as it only measures the average, rather than the blood sugar highs and lows throughout the day, which are often more important in determining the success of their treatment.
For cats being treated with an SGLT2 inhibitor, close monitoring is also important, especially during the beginning of the treatment. Bloodwork, including ketone levels and blood glucose curves, will be regularly monitored, as well as physical examinations and weight measurements.
Prognosis and Remission
Though there is no cure for feline diabetes, the prognosis for a good quality of life is good with adequate management at home. With early, aggressive treatment of diabetes, many cats will enter a state of diabetic remission, meaning they are able to maintain normal blood sugar levels without insulin injections. Older cats, cats who have previously received steroid medications, and cats treated with glargine insulin have been shown to be more likely to go into diabetic remission, but the most important factor is starting insulin therapy early and monitoring closely. If a cat has not entered diabetic remission within the first six months after diagnosis, it will almost certainly require life-long insulin injections. Cats who have achieved diabetic remission should continue to be fed a low-carbohydrate diet and receive close monitoring, as some will eventually require insulin therapy again.
Possible Complications
Insulin therapy and SGLT2 medications lower blood glucose, possibly to dangerously low levels. Signs of low blood sugar (hypoglycemia) include weakness, lethargy, vomiting, lack of coordination, seizures, and coma. Hypoglycemia can be fatal if left untreated, so any diabetic cat that shows any of these signs should be offered its regular food immediately. If the cat does not eat voluntarily, it should be given oral glucose in the form of honey, corn syrup, or proprietary dextrose gels (available at most pharmacies) and brought to a veterinarian immediately. It is important, however, that owners not attempt to force fingers, food, or fluids into the mouth of a convulsing or comatose cat.
Diabetic cats with uncontrolled diabetes may develop a condition known as ketoacidosis. This occurs when cells starved for glucose begin to break down fats for energy, a process that creates chemicals called ketones, which make the blood more acidic. Ketoacidosis is considered a medical emergency, and cats diagnosed with this complication require hospitalization for ideal management.
Monitoring Your Cat At Home
Monitoring a diabetic cat at home requires careful attention to a few things. Cats with well-controlled diabetes should maintain a normal activity level and demeanor. Owners should also monitor daily water intake, urine production, appetite, body weight, amount of insulin or medication administered, and possibly blood or urine glucose levels. Monitoring is best coordinated in close collaboration with your veterinarian to achieve optimal control over your cat’s diabetes.
Updated 2024