Pre-made immune memories could revolutionize immunization
Memory T-cells respond to fight specific pathogens.
New research suggests that our cells might not always need to be taught how to ward off pathogens. Instead, Cornell scientists believe that our bodies are born more ready than previously thought. With the potential to revolutionize how we immunize, findings published in the Cutting Edge section of the Journal of Immunology in March show that small populations of pre-programmed immune cells can fight specific pathogens they have not yet encountered. The researchers demonstrated a way to grow these cells, potentially transforming our approach to preventative medicine for infectious disease.
When first exposed to a new pathogen, the immune system takes up to a week to effectively respond and up to a month to make specialized memory cells that remember how to fight it. The next time a body is exposed these memory cells take care of it within hours. Scientists thought memory cells only developed after exposure until Dr. Avery August’s immunology lab found small pre-existing (innate) populations in 2008. But their defensive potential remained unknown until the latest study found they act exactly like memory cells that learn from exposure.

chair of microbiology
and immunology
“These fully-functioning innate memory cells open amazing opportunities for improving how we immunize,” said August, chair of the department of microbiology and immunology at Cornell’s College of Veterinary Medicine, who oversaw the study. “We’ve found a way to make millions of working memory cells without ever having to expose the body to a pathogen. If we can mobilize these cells to our advantage we can immunize much more quickly and eliminate the rare side effects of traditional vaccines.”
Vaccines work by stimulating memory cell creation, currently by exposing the body to a particular strain and waiting for the immune system to learn to respond. Making memory cells directly could eliminate that learning curve, letting people bypass booster shots and some slower-acting vaccines. People preparing to travel abroad could get immunizations the day before instead of planning weeks in advance.
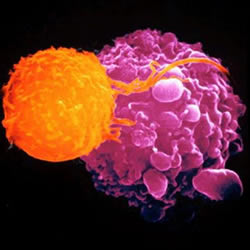
killing a cancer cell (mauve)
Our bodies normally have about 100 innate memory cells, but the body needs about 100,000 to defend against the average invader. Using bone marrow chimeras, a specialized transplantation technique, they were able to make 10 million. The study focused on memory cells designed to attack Listeria monocytogenes, bacteria that cause food poisoning, but August believes the model could be expanded to boost defenses against other infectious diseases.
“Theoretically we could generate memory cells for any kind of pathogen,” said August. “It looks like our immune systems are already trying to do this. The existence of these pre-made memory cells suggests that, over evolutionary history, our immune systems are trying to anticipate the pathogens we’ll face. Now we’ve found a way that could quickly help them along to improve immunities.”





