Equine Anesthesia: Keeping horses sleeping easy
This is an accompanying article to a Cornell Equine Seminar presented on Oct. 18, 2022 by Dr. Stephanie Hon, assistant professor of anesthesiology.
Anesthesia is a key part of many medical procedures – and one that carries inherent risks. Board-certified anesthesiologist Dr. Stephanie Hon explains different types of anesthesia and how owners can help their horses have the safest and most pain-free experience possible.
What follows here is an overview. Please watch Hon’s entire presentation for more extensive information.
What is a boarded anesthesiologist?
Anesthesia carries inherent risks. For horses, the morbidity and mortality rate is 1 in 100 for elective procedures and 1 in 10 for emergency procedures. The level of specialization and experience of the person performing the anesthesia greatly impacts how well these risks are mitigated.
“There’s no safe anesthesia, there are no safe anesthetics, there are only safe anesthetists,” Hon summarizes.
Boarded anesthesiologists (of whom there are only about 500 around the world) undergo a rigorous training at sanctioned institutions beyond their D.V.M. to help provide the highest level of care.
While anesthesia can be performed safely without a boarded anesthesiologist on staff, “three years of specialty training guarantee that there is an expert on hand to assess and mitigate anesthetic risks, to be at the cutting edge of anesthetic and analgesic drugs, and to know what the standard of care for monitoring of your patient is,” Hon says.

Medical history
Safe anesthetic care begins before the procedure. Owners can help by providing an accurate, thorough medical history for their horse, either directly in conversation with the anesthesiologist or through their primary veterinarian.
Because pre-existing conditions can impact the horse’s reaction to anesthesia, Hon emphasizes the importance of letting the anesthesia team know of any injuries and disorders.
Conditions that frequently change how the procedure needs to be managed include:
- hyperkalemic periodic paralysis (HYPP), a genetic disease that causes muscle tremors and weakness and under anesthesia creates an additional risk of such complications as airway obstruction.
- recurrent airway obstruction (RAO, or heaves), which can make ventilation under anesthesia difficult.
- lanryngeal paralysis, which may complicate inserting a tube into the airway.
- previous surgeries such as for prior fractures.
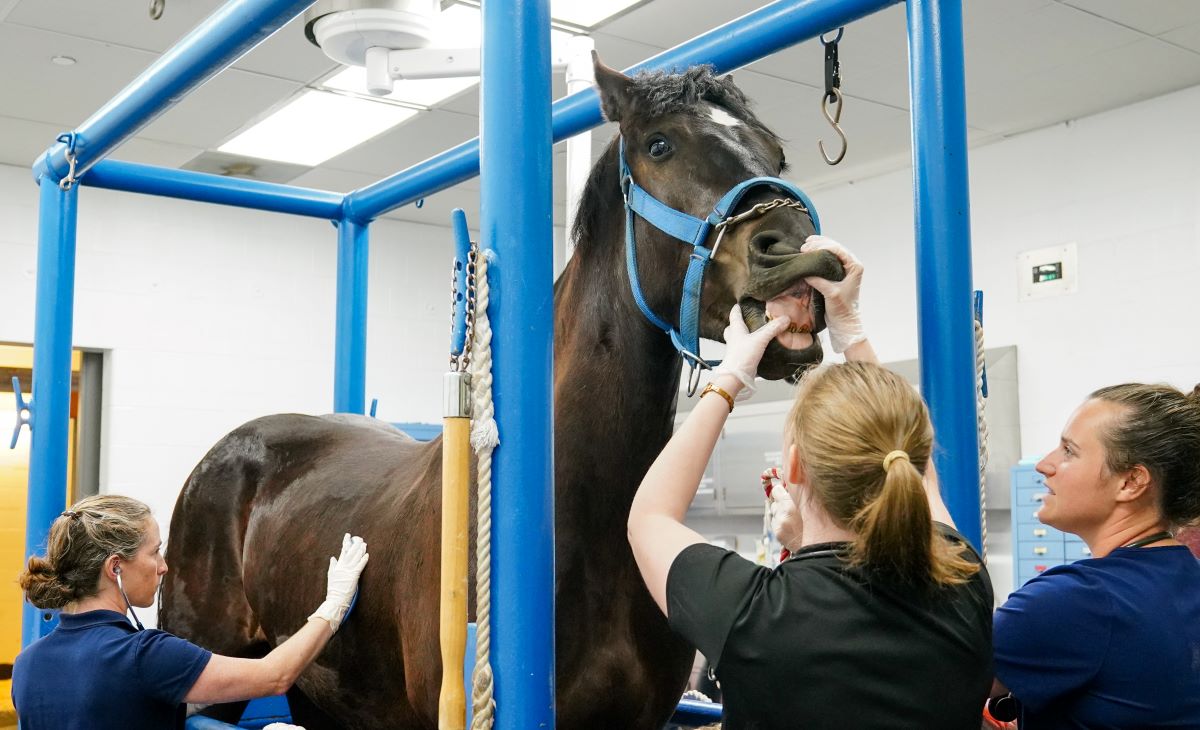
Pre-anesthetic exam
Next, the anesthesiologist will thoroughly assess the horse’s current condition.
During a physical exam, “we put our hands on the horse, we listen to them,” Hon says. The team evaluates all body systems, such as the heart, lungs, and musculoskeletal system, and notes any abnormalities.
Blood work checks the horse’s hydration status and other factors such as electrolyte balance, oxygenation of tissues, and underlying infection.
If advanced diagnostics are required, the anesthesiologist will order additional exams from other services to check the cardiovascular or respiratory systems.
Types of anesthetic management
Anesthesiologists choose between general anesthesia and standing sedation for any procedure. Each has its own risks and benefits:
- General anesthesia: Patients are given drugs to induce loss of consciousness and can’t be aroused, even by painful stimulation.
- Standing sedation: Patients’ consciousness is only depressed through drugs, so they cannot be easily aroused but can respond purposefully to stimuli.
Whenever possible, and if the horse tolerates it, standing sedation is preferable because it avoids the recovery period of general anesthesia, where most mortality and morbidity occur.
General anesthesia is most often required for scoping large joints for a significant amount of time or for advanced imaging with CTs or MRIs.
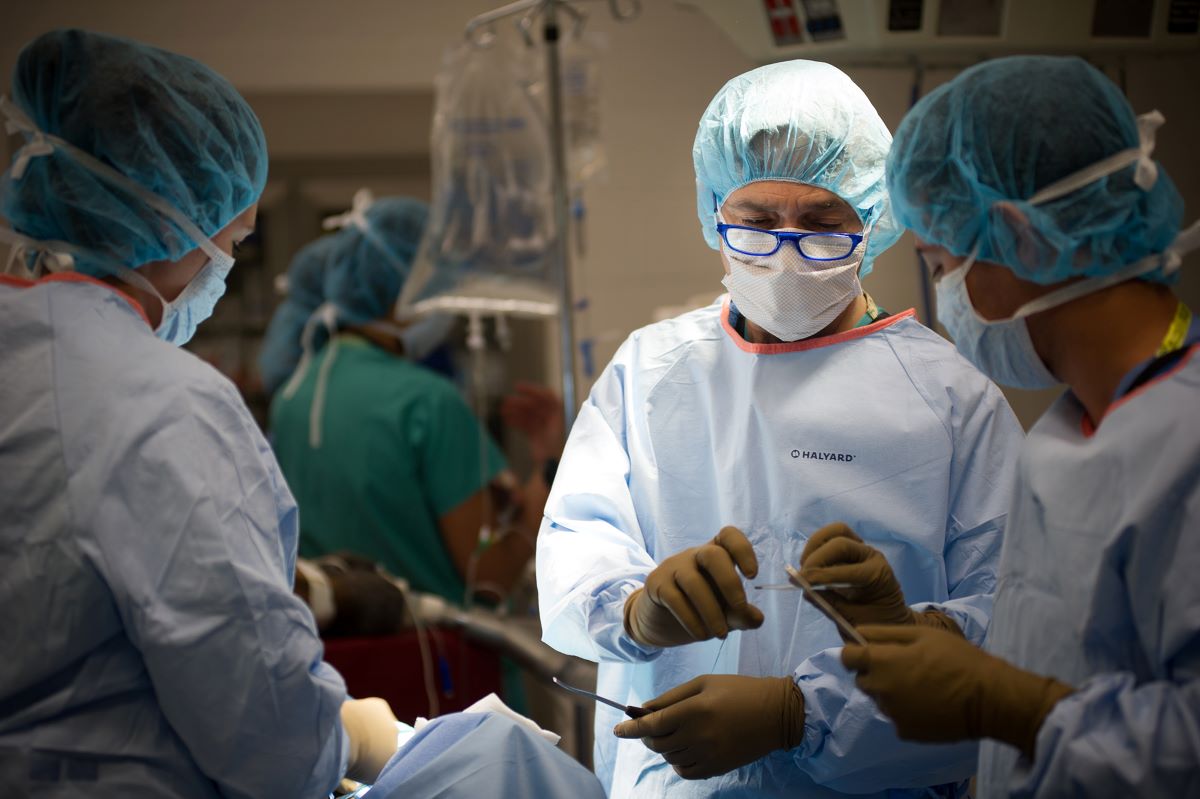
General anesthesia
On surgery day, a horse cleared for general anesthesia is led into the induction area. There it gets a final heart check to make sure it can safely receive the drugs.
After sedation, the team cleans the horse’s mouth in preparation for intubation and places head and tail ropes. Three to four people hold the animal against a wall and help guide it to the ground as the drugs – introduced through an IV catheter – take effect. The unconscious horse is hoisted in the air and lifted onto a table.
“Once we anesthetize the horses, we take over all of their body systems for them,” Hon explains. A breathing tube administers more drugs through the lungs and provides respiratory support with a ventilator, because the horse’s size and position on the back make it difficult for it to breathe appropriately.
Multiparameter continuous monitoring keeps track of heart, lung, and kidneys. “And we try to optimize their muscle perfusion, because they're going to have to go through a very athletic event of recovery at the end of all this,” Hon says.
The anesthesia team will choose the method of recovery that best fits the horse’s temperament and size, the staff’s training, and the available facilities.
Assisting a full-grown horse with head and tail ropes inside a box is the riskiest approach for the two staff members involved. Foals will not tolerate ropes but are light enough to assist safely by hand. Applying head and tail ropes from outside the box strikes a good balance between the needs of the horse and staff safety, though more people are required. Some horses also do well with free recovery, without assistance.
In all cases, monitoring and recording recoveries with cameras as part of the medical record is becoming the standard of care.
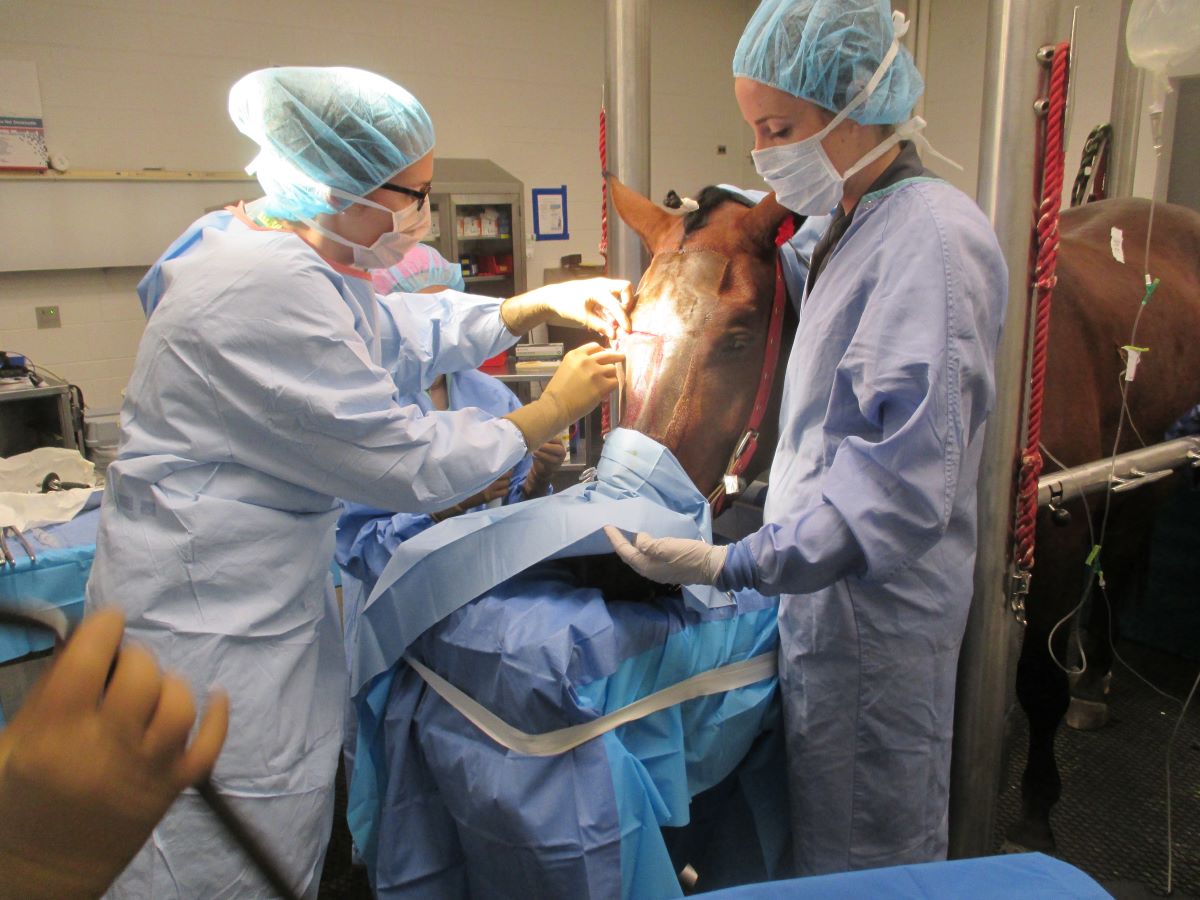
Standing sedation
In contrast to general anesthesia, standing sedation with continuous injectable anesthetics keeps horses at a level that lets them tolerate any stimulus from the ongoing procedure. It involves only basic heart rate monitoring and no recovery.
Ready for surgery, the horse stands in a stock and may receive ear puffs and a urinary catheter to help create a stable environment for both patient and surgeon. “Those are all things outside of the drugs that anesthesia can help with in order to maintain the horse,” Hon explains.
Standing sedation is a good option for older horses for whom recovery would be very difficult or for patients undergoing surgeries that in the past resulted in high morbidity and mortality under general anesthesia. “If we can do a procedure standing, we’ll elect to do that,” says Hon, noting that this form of anesthesia is suitable for a growing number of interventions, such as many airway surgeries and most dentistry and urogenital surgeries.
Locoregional anesthesia
To ensure that a horse is conscious enough to remain standing but does not feel pain beyond the level of sedation, anesthesiologists can desensitize only a region of the body (regional anesthesia), such as the perineum or hindlimbs, or a specific area of the body (local anesthesia), such as the limb that has a laceration. “This can be a really powerful adjunctive therapy to use in addition to your sedation,” says Hon.
She stresses the importance of starting the analgesia before surgery begins and before the body registers pain that can upregulate the pain receptors, making them more sensitive.
Boarded anesthesiologists are deeply trained in applied anatomy, so they are particularly skilled in safely placing the nerve blocks without damage to surrounding tissues. For example, an anesthesiologist may use a special blunt needle to target the maxillary nerve to block sensation from all cheek teeth and some sinuses, avoiding laceration of a neighboring artery and bleeding that could put pressure on the eye. “That’s one nuance where someone who is boarded will be tuned not only into the steps they have to do but all of the ramifications of what this procedure might entail and how we can best use this block,” Hon explains.
Advanced pain management
Anesthetic management of the patient begins before surgery and does not stop at the operating theater.
Chronic pain, for example, turns on many pain receptors. An anesthesiologist may start a horse on pain therapy and management well before the procedure so its pain sensors quiet down enough for the animal to tolerate the added stimulus from surgery.
After the procedure, anesthesiologists will continue to treat pain and inflammation that may persist up to 72 hours in the tissues that have been handled. One advanced technique they use is giving continuous doses of pain medications through an epidural catheter at the end of the horse’s sacrum. “We can redose it as needed, consult with the primary service, taper them off, and help pain score them, so that their post-operative or recovery period can also involve some advanced analgesics,” Hon says.

Innovation in the field
A tertiary referral hospital such as the Cornell University Hospital for Animals brings together anesthesiologists who are on the cutting edge of their specialties. “So a nice facet of the academic environment is that we’re tasked with the development of new techniques and new paradigms of thought all the time,” Hon says. Faculty members have developed many innovative surgical techniques.
At the same time, Hon says, Cornell’s anesthesiologists are happy to speak to owners about their horses and consult with other practitioners on challenging cases. “We really welcome the chance to be part of the holistic team taking care of our patients.”
Watch Hon’s full talk online, and see the entire Cornell Equine Seminar Series videos here.




