Common Dental Procedures and Pathology
Regional Nerve Blocks:
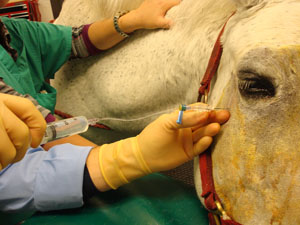
Providing adequate pain control for equine patients in the perioperative and postoperative period should be part of any practitioner’s surgical plan involving dental extraction and/or sinus surgery. The vast majority of extraction techniques in common use today can be performed standing with good perioperative analgesia/anesthesia via intravenous sedation and regional nerve block. This greatly reduces the risk to the horse from general anesthesia, bleeding during surgery and recovery time. Many same day surgeries can be performed with only a 48 hour stay at our equine hospital.
One facet of a good multimodal pain control plan is regional nerve block. Nerve blocks are the key to being able to perform dental extractions in the standing horse under a constant rate intravenous infusion of an anesthetic agent. Prior to the common use of regional nerve blocks for standing extractions, the surgeon’s success relied more on the nature of the horse, very high doses of intravenous anesthetics, and uncomplicated or nonsurgical extraction procedures. With the use of nerve blocks now most horses can have productive noninvasive and invasive dental procedures standing. General anesthesia is still necessary for intractable patients, surgeries requiring computed tomography, and extractions or maxillofacial surgeries requiring precise, delicate surgical technique. When placing a nerve block achieving effectiveness while reducing risk is paramount. Three common regional nerve blocks used for dental procedures are the maxillary, middle mental, and inferior alveolar nerve blocks.
Dental Imaging:
Diagnostic imaging is a critical tool for complete evaluation of oral health and disease in the horse. Even the most advanced oral exam using endoscopic techniques will not be able to determine the health of adjacent hard and soft tissue structures, the reserve crown, and the roots located within the alveolus. Some equine teeth that appear normal on examination of the clinical crown can be the cause of regional sinusitis, impressive apical pathology, and fistula formation. Diagnostic imaging can help identify the tooth/teeth responsible for current clinical signs as well as provide additional information regarding the health of otherwise clinically normal teeth. Many times incidental pathology can be identified during imaging studies allowing the veterinarian to diagnose the current problem and to warn the owner of developing pathology.
The first step in evaluating any horse for dental pathology should be a complete oral examination. Over the past decades, advances in intraoral imaging have made the exam more fruitful. The introduction and emphasis on using a mirror to evaluate teeth intraorally was followed by suggestions for the use of an intraoral camera. Rigid endoscopes have proved most useful, and there are currently a handful of models to choose from on the market. At Cornell, our rigid endoscope detects subtle lesions on the tooth surface and in adjacent soft tissue that was previously invisible to the practitioner. It is also a valuable teaching tool for students and clients as they are able to view the pathology in real time.
Radiology is widely used for dental imaging, and the combination of view variety and improved imaging systems has led to a renaissance in the practitioner’s ability to diagnose pathology with this modality. With the appropriate tools, adequate views, and experienced eyes, the majority of dental cases can be diagnosed with a complete oral examination and dental radiography. When radiography is not enough, four additional modalities can be utilized to provide additional information. Ultrasound, nuclear scintigraphy, magnetic resonance imaging (MRI), and computed tomography (CT) have all been used as ancillary techniques to either confirm or complete a diagnosis. CT has proven to be the most valuable of these four modalities to identify maxillofacial and dental pathology providing accurate images in cross sectional and multiplanar views. Both soft and hard tissue algorithms with or without contrast provide ample information. Three-dimensional reconstructions are particularly useful for maxillary and mandibular fracture repair.
Equine Odontoclastic Tooth Resorption and Hypercementosis (EOTRH):
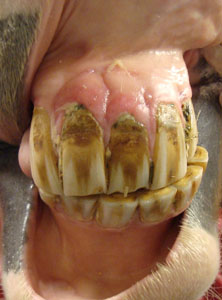
EORTH is a newly recognized pathology affecting both the incisors and canine teeth of the horses typically greater than 15 years of age. EORTH is characterized by internal and external resorption of dental structure sometimes associated with excessive production of cementum on the exterior of the tooth. As the disease progresses, the pulp, periodontal ligament, and alveolar bone become inflamed and infected leading to reduced structural support for the teeth, degradation of gingiva, increased incisor angle, fistula formation, tooth fracture, and pain.
EORTH in general is a painful disease. The most common initial sign of incisor pain reported by owners is a reduced ability in grasping apples and carrots. Many horses over time will eventually become completely disinterested in accepting these treats. Other signs of pain associated with EOTRH include sensitivity to biting, head shaking, ptyalism, resistance to turning during work, shyness about the head, periodic inappetance, weight loss, and decreased use of incisors for grasping and grazing. Some horses become incredibly adept at grasping feed with the lips, sliding it past the incisors and moving it into the mouth through the “bar” region. Watching how an EORTH horse eats hay prior to an oral exam is a good way to gauge the animal’s discomfort and stage of disease. Some highly trained horses or horses in earlier stages of the disease can show no apparent signs of discomfort, and patients with primarily hypercementosis and very little to no resorption also seem to remain comfortable. Oral exam can be quite challenging because patients are resistant to manipulation of the lips and pressure on affected teeth. Placement and opening of an oral speculum can elicit alert and possibly dangerous behavior even under heavy sedation. Oral exam findings can include enlarged mandibular lymph nodes, decreased incisor angle not appropriate for age, prominent juga, loss of dental papillae, gingival and mucogingival fistulas, severe regional inflammation, purulent drainage, calculus and feed accumulation, missing teeth, hyperplastic gingiva, gingival recession, bulbous enlargement of dental structures, tooth mobility, and supragingival regions of dental resorption. Resorptive lesions in older horses can be found under excessive tartar deposition on the mandibular (more common) and maxillary canine teeth. Exposing these lesions after removal of tartar will cause discomfort for the horse and the practitioner should be prepared to address the problem either through extraction under primary care or referral to a dental or surgical specialist.
EOTRH necessitates intraoral radiographs of both the incisors and canines to properly formulate a treatment plan. Radiographic findings typically include loss of the periodontal ligament space, disruption of alveolar and regional cancellous bone, osteomyelitis, and tooth fracture. Cases involving only hypercementosis can usually be monitored via annual oral exam and radiographs as these horses usually remain comfortable for a long period of time. Patients with mild subgingival resorption and no regional osteitis or alveolitis can be monitored with oral exam and radiographs as the pace of disease progression varies between teeth and individuals. It is not uncommon to see on radiographs a variety of disease stages ranging from normal to severe throughout the incisors and canines. Once supragingival lesions, alveolitis, osteomyelitis, tooth fractures, and extensive resorption of the reserve crown and root are detectable on radiographs extraction is recommended. Moderate to severe cases of EOTRH require staged or complete extraction of the affected incisor and canine teeth to alleviate infection and pain caused by this disease. Incisor extraction can be accomplished in two ways depending on the nature and severity of the pathology associated with the tooth/teeth. Singular incisor extraction can be accomplished simply in mild to moderately affected teeth by elevation and avulsion. In cases of multiple incisor and canine tooth extraction with severe EOTRH, a surgical approach is necessary to allow for complete removal of dental material, visualization of tooth and diseased structures, debridement, and closure. In addition, a surgical approach increases the surgeon’s ability to deal with complicated extractions where reserve crowns and roots have fractured due to initial trauma and resorption.
Post-operative radiographs are recommended for every extraction procedure to ensure no dental fragments have been left behind and to provide documentation of the procedure and lack of adjacent hard tissue damage. Post-operative pain medication and antibiotics are indicated in surgical extraction procedures. Owners should be instructed to keep horses on a pelleted mash for the first 12 hours. After this time, soft soaked hay, dengi, or soaked hay stretchers can be introduced with dry pelleted feed. The surgical sites should be rinsed with warm water or a warm antimicrobial rinse (0.12% chlorhexidine or very dilute betadine) twice a day until the sutures fall-out or are removed. Most horses will return to a hay diet, but some older horses may need supplementation with a senior pelted feed to maintain weight. Some horses will also continue to graze, but it should not be assumed that they can maintain a normal energy intake on pasture alone and should be have hay available.
It should be noted that mucogingival flaps in horses are notorious for dehiscence especially on the mandible. The reason behind this is not exactly known, but time devoted to mastication, disruption of circulation during surgery, labial and frenulum attachments, gravity and tongue action have all been thought to contribute to dehiscence. Dehiscence if present usually occurs between days 5 – 10, when granulation tissue, partial primary closure, and wound contraction have already started to occur at the surgical margin. Sutures involved with the dehiscence are removed, and the owner is instructed to flush the wound twice daily with an antimicrobial rinse until complete healing has occurred by second intention (usually 2-5 weeks). After the removal of all incisor teeth, it is also common for the tongue to protrude slightly from the oral cavity on a routine basis due to the loss of incisor retention. The horse does maintain the ability to fully retract the tongue in the mouth, so there is no incidence of secondary trauma or desiccation of the tongue….just an endearing smile!
Dental Extraction:
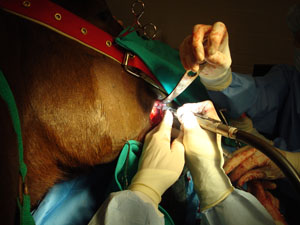
Pathology associated with equine cheek teeth has been well documented by many research veterinarians and scientists from around the world. Dental fractures leading to significant crown loss and pulp exposure, apical infection, periodontal disease, dental malformation, supernumerary teeth, and maloccluded teeth are all potential pathologies that would necessitate extraction of a cheek tooth. Patient age and health, severity of disease, tooth positioning, severity of clinical signs, and owners financial and physical capabilities all play a role in determining if extraction is the best therapeutic option. Extraction of equine cheek teeth, especially of those that are not already mobile, is a demanding undertaking for both horse and veterinarian. Extraction requires proper sedation/anesthesia, analgesia, visualization, specialized equipment, and assistant help.
In all published studies to date, intraoral extraction of teeth has provided the highest success rate and the lowest complication rate of any extraction technique; therefore, intraoral extraction of cheek teeth in the horse is always be considered prior to surgical extraction options. Surgical extraction techniques are an excellent option for all cheek teeth where other extraction techniques would prove impossible or less ideal for the diseased tooth and horse. The fact that there are so many different approaches to the extraction of equine cheek teeth highlights that no one technique is appropriate for every case. Indications for surgical extraction are loss or severe damage to clinical crown, tooth resorption, hypercementosis, ankylosis, crown-root fractures, apical infection of young teeth, impacted teeth, open-mouth restriction, very small patient size, radicular/odontogenic cyst formation, oronasal fistula involvement, and dental malformation.


