Scientific collaboration yields link between bariatric surgery and colitis
For decades, bariatric surgery has been one of the most effective long-term treatments for obesity. This has made bariatric surgery an increasingly popular procedure, with over 200,000 patients undergoing this surgery per year in the U.S. However, it is not without its risks. There have been conflicting reports on the effect of bariatric surgery on Inflammatory Bowel Disease (IBD), including colitis and Crohn’s disease, with some recent reports suggesting that bariatric surgery increases the risk of IBD.
CVM researchers Dr. Bethany Cummings and Dr. Praveen Sethupathy ’03 in the Department of Biomedical Sciences collaborated on a study that teases out the connections between bariatric surgery and IBD, recently publishing those findings in the journal “Obesity Surgery.” Cummings has been developing and studying mouse models of bariatric surgery to understand the positive and negative effects of these surgeries for years. Sethupathy is an expert in gene regulation and microRNAs, particularly in the context of gastrointestinal health and disease. Therefore, they combined their expertise to gain clarity on the effect of bariatric surgery on IBD.
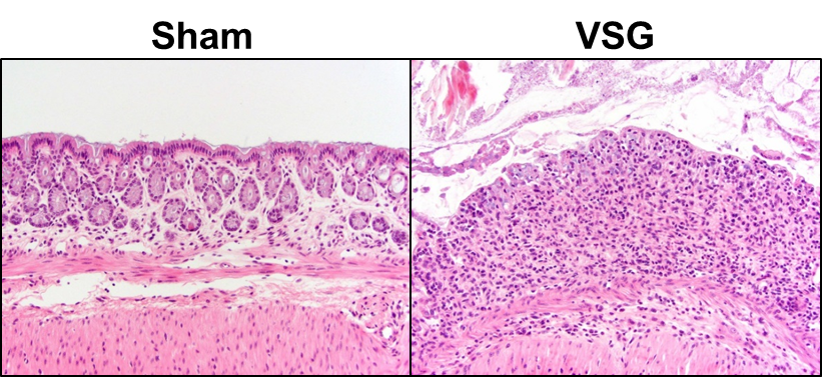
Vertical sleeve gastrectomy (VSG), the most common type of bariatric surgery, increases bile acid concentration and the subsequent signaling of the bile-acid receptor TGR5. In previous mice studies, researchers found that an uptick in TGR5 signaling will protect mice against colitis. By this logic, VSG patients should have less incidence and worsening of colitis—yet this isn’t always the case.
To understand the interplay between VSG and TGR5 signaling, the Sethupathy and Cummings teams compared mouse models that had received VSG with those that underwent a sham surgery, while also comparing mice with and without the TRG5 receptors. Each of these groups were given chemically-induced colitis to determine how the disease progressed under each of these conditions.
As the researchers expected, the mice that had their TGR5 receptors genetically knocked-out suffered from worse colitis symptoms than the controls. More surprising, though, was the fact that VSG-treated mice with TGR5 receptors intact still suffered from colitis, despite the fact that those mice had higher bile acid signaling through the TGR5 receptors. “Our data suggest that VSG worsens the severity of experimental colitis, which may explain the increased incidence of IBD development observed in human patients after bariatric surgery,” says Cummings.
The researchers theorize that this may happen in part due to the dramatic alterations in gut microbe make-up after bariatric surgery. “The changes in the gut microbial composition after bariatric surgery are very similar to changes seen in human patients suffering from IBD,” says Cummings. Another key player could be a specific microRNA known as miR-21. “We have shown previously that this microRNA is among the most aberrantly elevated in the colon of human patients with IBD,” says Sethupathy. In this study, Cummings and Sethupathy have found that this microRNA is also significantly elevated after VSG in mice. They posit that post-operative increases in colonic miR-21 expression may promote tissue injury and the risk of colitis development. “Other recent studies have linked miR-21 to the control of gut microbial composition, but whether that is relevant in the context of VSG remains to be seen,” says Sethupathy.
The findings from this latest study provided the basis for a multi-PI NIH R01 grant application that Cummings and Sethupathy submitted last fall — if awarded, the grant would allow them to determine the precise mechanisms by which bariatric surgery promotes IBD. “The hope is that this research will allow us to develop prophylactic treatments for this rapidly expanding population of patients undergoing bariatric surgery to help prevent the development of IBD,” says Cummings.
By Lauren Cahoon Roberts



